The Ultimate Breastfeeding Guide
Breastfeeding is one of my most favorite things to do. It is the most absolute sweetest and most tender moment that you can endure with your newborn baby. However, sometimes, it is not all nice and cozy as it may seem.

In the beginning, I was so fed up that I cried and cried. I thought that I sucked at breastfeeding and told my husband over and over that I was for sure quitting-but, I didn’t of course. I just had so many issues with it and I wanted to take the easy way out and say, “Why bother?”
Why bother? Oh man, there are way too many benefits to reply to that question!
Breastfeeding:
- Increases your bond with baby
- Reduces your chances for breast cancer
- Burns up to 500 calories daily (yay!)
- Saves you money because its free
- Is Convenient
- Lowers the risk of childhood issues such as ear infections, asthma, and eczema
- Reduces your chance of developing Type II Diabetes later in life
- Also reduces your chances for ovarian cancer
- Is better for the environment
- Can make your baby stronger by strengthening his or her immune system
- The list goes on, people…
I toughed it out and by the 3rd month, I had things perfectly down and felt a whole lot more secure in my breastfeeding skills. I no longer got frustrated, I no longer cried, and I no longer made dumb ramblings of how I was going to quit and so forth.
I hope this information helps you as much as it has helped me. I am 38 weeks pregnant and still nursing my two year old son and I plan to tandem feed both him and my daughter once she is born!
Latch On!

When I first started breastfeeding, it was a nightmare. No, really. My son lost around 11 oz. by his 48 hour hospital check because we were having issues with latching on. Did you know that over 50% of women experience difficulty with the latching on process and, in general, breastfeeding? I did not believe that until I went through it! I was so excited to breastfeed and thought it would be so easy. Boy, was I wrong!
I decided to meet with the lactation consultant at our local hospital ASAP to correct the problem because my son would not latch on at all-and I did not want to turn to a bottle. I met with her and I cried and expressed my fears and frustrations. I told her that I felt like a total failure. She smiled and knowingly told me “This is very common.”
She had me take out a boob and demonstrate on my son how I attempted feeding him at home. She immediately caught my issue-the latching and that I was being too relaxed in my role as the breastfeeder. She told me I had to almost manhandle my son to guide his mouth to the nipple. She said, “Don’t be afraid. If you do not show him, how will he ever learn?”
I used a little force to guide my son’s head to the nipple using the technique I learned in breastfeeding class. You want the entire areola (or most of it) inside your baby’s mouth as they suckle. I have actually heard of some lactation consultants telling women that your areola shouldn’t even be visible!
This means a baby tips his head back slightly and leads with his chin and lower jaw, taking more areola below the nipple than above; this also results in the nose being clear of breast tissue. (If baby’s mouth is aligned with the nipple, you will then have to squeeze/shape the breast to obtain effective attachment and avoid a symmetrical latch.)
Here is a great picture example from La Leche League:
A good latch:
- Enables your baby to suckle effectively
- Prevents sore, cracked, painful, or bleeding nipples
- Prevents baby from tugging at the nipple in order to gain more access to your milk supply.
Signs of a good latch are:
- Cheeks are rounded
- Mom can hear the baby swallowing
- The ears move
- Baby falls off the breast after feeding, or is very relaxed after feeding
The lactation consultant then told me to go home, have a small glass of wine, and RELAX. She told me that my newborn could feel my frustration and stress, which was effecting him latching on-and my milk supply! Who knew, right? So I did just that. And guess what? I became a badass, confident breastfeeder!
Here are some very helpful tips that have personally helped me cope with my breastfeeding woes:
- Bring baby to the breast-not vice vera. Before knowing this, I would arch my back and hunch over my baby-which resulted in a poor latch and a back ache for me!
- Wait at least 3 weeks before introducing a bottle to allow your baby to get used to the breast.
- Make sure baby’s mouth is opened wide before latching. Too small, and he will only latch onto your nipple-ouch! To get him to latch touch your nipple to his upper lip and wait for him to open up.
- Make sure your areola is covered by his mouth. Sucking on the nipple does not stimulate letdown like the areola does.
- When attempting to latch on, hold your breast in with your hand in a U shape. This will make it easier for him!
- To boost your milk supply, eat oats and drink lots of water! Seems like a simple tip, tried it, and its true!
- Abuse that Lanolin cream! Use it after every feeding! It is your friend.
- Baby can sense your tension if you are anxious and stressed. Make sure you are comfortable before setting up to feed.
Did you know that there are multiple positions and ways that you can breastfeed your baby? My personal favorite is a lying position since my son is weighing in at 21lbs ever since he was 6 months old! Also, it is very calming and relaxing to me!
Here are a few positions to choose from, but are not limited to:
Football Hold
Cradle Hold
Cross Cradle Hold
Laying Down
Laid Back
Find the position that best suits you and go with it!
However, if I could go back in time, I would have switched up my positions more because my son became so used to strictly breastfeeding while laying down, that he would barely breastfeed in any other position!
Pump Away!
My pump was seriously my B.F.F. Like, seriously.
I started pumping as soon as I came home from the hospital-on the 3rd day-which is pretty much when my milk decided to come in at full force! BAM! Never had I ever had such large breasts-I did not know what to do with them. My son would feed a little on both breasts and pass immediately out like a light bulb and my boobs were still full. This is where the pump came in handy.
So, what are the benefits of pumping, exactly? Some are:
- Less of a chance for sore nipples
- Knowing exactly how much your baby eats in one sitting
- It could be more convenient for you, depending on your situation
- This leaves an opening for others to offer to feed baby when you need a break
- You burn as many calories when you pump as breastfeeding.
- Your baby still reaps the benefits!
- You can keep up your supply even if you work outside of the house
I know what you are thinking: “Where the hell do I start? What are the best pumps available?”
My personal favorite pump has been anything from Medela! I currently own the Medela Pump In Style Advanced and the manual Medela pump and have had them since day one. But, this might be due to the fact that I honestly have not tried any other brands on the market.
However, I did do a ton of research during my pregnancy and talked to about a zillion mothers who were veteran pumpers and Medela was the way to go. I am so happy I chose this brand (no endorsement, just love it). But as long as you have a good pump that: 1) works efficiently 2) doesn’t rip your nipple off and 3) is durable then you are good to go!
I will recommend that you should have one manual and one electric-because the electric pump makes life so much easier-especially when you milk comes in! Trust me, you’ll get hand cramps.
Here is a list of the top rated pumps to choose from. Please keep in mind that are tons of different brands and not everyone is going to like the same pump. Find the pump that best suits you! Don’t like it? Return it and try another one!
Medela Pump In Style Advanced Double Electric Pump ($270): This pump has a durable motor, a battery pack for times you can’t find an outlet, “letdown” mode that helps get the milk flowing, and adjustable settings. This double electric pump is pretty much a working mom’s best friend!
Dr. Brown’s Double Electric Pump ($150): This electric pump is said to be the most comfortable pump on the market because its suction cups are extra soft and moves to mimic a baby’s tongue motions.
Lansinoh Affinity Double Electric Pump ($120): Unlike, the Medela, this pump comes with a less hefty price tag for those who rather not spend over $200 on a breast pump.
Medela Manual Pump ($30): A single manual pump comes in handy for relieving engorgement or providing the occasional bottle for baby. It’s good for travel, too, since there’s no battery or electricity needed.
Phillips Avent Manual Pump ($40): This is yet another top rated manual pump on the market. This pump is said to be absolutely comfortable featuring a massage cushion as you pump.
Lansinoh Manual Pump ($25): This pump is said to be one of the best pumps on the market for its low price. If you are on a budget, this is the one you want!
Luckily, for the first 6 months of my son’s life, I worked hard to build my milk stash. I even had to purchase a deep freezer! I would pump maybe 3-4 5oz bags per day of milk!
Lots of mothers want to know how to build a stash and pumping is one way to do it. I will go into building your stash soon.
Here are my favorite tried and true tips that have helped me while pumping:
- Pump OFTEN. I was personally either feeding OR pumping every TWO HOURS for the first 6 months straight. I never skipped a beat. Even at night. I pumped 1-2 times throughout the night alternating with feeding.
- I ate a ton of oats! Oatmeal, granola bars, you name it. Oats are known to boost lactation.
- Get a good breast pump. The best out there and the one I use is the Medela Electric Double Pump. It pumps both breasts at once and is mighty powerful! It pulls all of the milk out, allowing my breasts to completely empty (a common issue).
- When you pump, check out your technique. Do not forget to compress or squeeze your breasts. Sometimes the milk ducts get plugged. By squeezing your breasts, it helps to lure the milk out.
- Try warm compresses for 15 minutes before your pumping session. This will not only ensure lots of milk, but help the milk to flow easier and faster.
- Massage your breasts to avoid cysts from forming.
- Make sure your nursing bra is SUPPORTIVE. Most women wear the WRONG SIZE.
- Use Bamboo nursing pads to protect your nips.
- DRINK WATER!!! In order to make milk, you need H20!
- Eat a good diet with ENOUGH calories. 500 calories a day is what breastfeeding burns so EAT THEM BACK!
- Use lanolin. This will act as a barrier and moisturizer for your nips!
- Stock your milk. You never know when you might dry up.
Common Breastfeeding Myths
When it comes to nursing, I am sure that you have heard a thousand do’s and don’ts to the point where you are probably wondering what the hell is fact and what’s fiction. A lot of it honestly varies from person to person; however they usually stay the same.
Here are a few of the most common myths and the truths behind them:
MYTH: You cannot breastfeed with implants.
FACT: This is not true for many women. I breastfeed with my implants and it is absolutely fine! I chose to go the submuscular route so that my mammary glands would not be effected or cut into. However, on the flip side, some women are not able to breastfeed with implants because they went the subglandular route or somehow the surgery damaged their nerves, breast milk ducts, or milk glands. Where and how the implant is inserted has everything to do with the likelihood the woman will be able to breastfeed in the future. If you avoid a nipple incision and instead put the implants under the breast crease – a procedure called an inframammary incision – or if you put the implants under the muscle of the chest wall, the majority of patients do not have a problem breast feeding.
MYTH: Pumping is a good way of knowing how much milk the mother has.
FACT: Not true! How much milk can be pumped depends on many factors, including the mother’s stress level. The baby who breastfeeds well can get much more milk than his mother can pump. Pumping only tells you have much you can pump.
MYTH: There is no way to know how much breast milk the baby is getting.
FACT: Not true! There is no easy way to measure how much the baby is getting, but this does not mean that you cannot know if the baby is getting enough. The best way to know is that the baby actually drinks at the breast for several minutes at each feeding (open mouth wide—pause—close mouth type of suck).
MYTH: The mother should not be a pacifier for the baby.
FACT: Comforting and meeting sucking needs at the breast is nature’s original design. Pacifiers (dummies, soothers) are literally a substitute for the mother when she can’t be available. Other reasons to pacify a baby primarily at the breast include superior oral-facial development, prolonged lactational amenorrhea, and avoidance of nipple confusion and stimulation of an adequate milk supply to ensure higher rates of breastfeeding success.
MYTH: Nursing babies shouldn’t take an occasional bottle or they may become confused and stop eating.
FACT: Babies suck on a nipple, but suckle at the breast. The difference between the two actions rarely will confuse your little one, says Sternum. If you think you need to supplement your baby’s feedings (particularly if you plan to return to work before you finish nursing), then you should introduce baby to a bottle between 2 to 6 weeks of age.
MYTH: It is normal for breastfeeding to hurt.
FACT: Not true! Though some tenderness during the first few days is relatively common, this should be a temporary situation that lasts only a few days and should never be so bad that the mother dreads breastfeeding. Any pain that is more than mild is abnormal and is almost always due to the baby latching on poorly. Any nipple pain that is not getting better by day three or four or lasts beyond five or six days should not be ignored. A new onset of pain when things have been going well for a while may be due to a yeast infection of the nipples. Limiting feeding time does not prevent soreness. Taking the baby off the breast for the nipples to heal should be a last resort only.
MYTH: Poor milk supply is usually caused by stress, fatigue and/or inadequate fluids and food intake.
FACT: The most common causes of milk supply problems are infrequent feedings and/or poor latch-on and positioning; both are usually due to inadequate information provided to the breastfeeding mother. Suckling problems on the infant’s part can also impact milk supply negatively. Stress, fatigue or malnutrition are rarely causes of milk supply failure because the body has highly developed survival mechanisms to protect the nursling during times of scarce food supply.
Setting a Routine
Setting some sort of schedule or routine for your nursing and pumping will make your days a whole lot easier. Did you know that infants actually thrive off of a set routine? Once you’ve created and implemented your plan and practice it daily, you baby will learn to catch on and expect the feedings at the designated times and, not to mention, your body will go along with it as well!
However, this can all be tricky when it comes to a newborn-and this is probably a good thing why maternity leave is anywhere from 6-12 weeks these days. When your baby is brand new, he or she hasn’t the slightest clue when on Earth they are going to get the boob. All they know is “I am hungry and I want it NOW!” So, there’s no routine going on in the beginning, its just simply supply & demand-this is normal. I actually wouldn’t suggest beginning a routine until the 6th week or so-that’s when we started our son on his and it worked out pretty well.
So, what routine did we use? The E.A.S.Y. method from The Baby Whisperer. I highly recommend this book-I am usually not a go-to-a-book-to-find-out-how-i-should-live-my-life kind of gal, but this thing was pure magic.
Here are a couple of samples of how my routines went, personally. Keep in mind, they did change a bit from month to month as he aged. But here was from about 6 weeks till 12 weeks. Also keep in mind that I am a work from home mommy-if you are working, then you can refer to chapter eleven of an idea for your typical pumping/feeding schedule.
Your baby’s routine will change from month to month. My advice? Roll with the punches and tweak your routines to best fit your baby’s needs.
**NOTE: Every baby feeds & sleeps differently. Do not get discouraged if they fail to conform to some sort of routine. It will eventually happen, but try not to force it. Just influence. **
Sample Breastfeeding Schedule (6-12weeks)
6am – Breast
10am – Breast
1pm – Breast
4pm – Breast
7pm – Breast
10pm – Breast
2am – Breast
My pumping routine from about 0-12 weeks was honestly pretty random. I pumped on demand-meaning, in between feedings while my milk was still coming in very greatly, I had to pump to relieve myself of engorgement. I would actually have to pump right after a feeding sometimes so that I could completely empty each breast since my son did not eat a whole lot during each feeding when he was younger.
My advice? Pump as needed.
Here is what my typical pumping day looked like from 6-12 weeks postpartum. As you can see, I usually would pump after a feeding to empty my breast completely.
Sample Pumping Schedule
6:30am- Pump
10:30am- Pump
1:30pm- Pump
4:30pm- Pump
7:30pm- Pump
10:30om- Pump
2:30am- Pump
Boosting Your Milk Supply
When it comes to the topic of breastfeeding, many women want to know how to keep up a healthy milk supply and to avoid going dry. We have already busted the myth that exercising does not decrease your milk supply and how you can keep your supply up while trying to lose weight and working out. I will go ahead and tell you that the #1 way to boost your supply is…. Drumroll….. PUMPING & FEEDING OFTEN! Your milk production is a supply & demand type of thing, you see.
It is also important that you calculate the amount of calories that your body needs to keep producing milk. There are certain foods have been proven to help many women from going dry by their lactogenic properties; you may even have a few of them in your kitchen already!
Here are 10 foods that have been proven to give your supply a little boost!
- Oats. Many moms have noticed that they had pumped more milk on the days they had oatmeal for breakfast than on days that they hadn’t. Though there is no proven scientific explanation, oatmeal is thought to be a calming food that helps you to release more oxytocin which boosts milk production. Oats are also a great source of iron; studies have shown that a low iron supply can decrease your lactation greatly! Oats are thought of so highly when it comes to breastfeeding that there are even “lactation cookie” recipes floating around with the prime ingredient being oats!
- Flax Seeds. Flax seeds are thought to have lactogenic properties because of the Omega 3’s that it contains. As mother’s breastfeed, their fatty acid stores are depleted within the milk that is being pumped or consumed by baby. Try adding some flax seeds to your morning oatmeal or to a smoothie for a quick boost!
- Brewer’s Yeast. This nutrient supplement is packed with vitamins & nutrients that are not only beneficial for breastfeeding, but also aids in postpartum depression and balances the immune system. It is specifically high in Choline which helps transport fat throughout the body and helps replenish the body’s cells to aid in new tissue development. You can cook with this nutritional yeast, add it to a drink mixture, or take it as a supplement in a tablet form.
- Water. Although water is not technically a food, it is vital to breastfeeding moms because as you nurse, your body becomes depleted of fluids. The more hydrated you are, the more milk you are likely to produce when breastfeeding. Aim for at least 8 glasses or 64 ounces of water daily.
- Spinach. This leafy green is packed with tons of vital nutrients and phytoestrogens. Phytoestrogens are believed to promote healthy breast tissue & lactation since this plant based chemical is similar to estrogen. Try adding spinach to your nightly dinners by making a side salad or to a green smoothie in the morning for breakfast.
- Garlic. Though garlic is not the most popular choice of lactation friendly foods, it has been shown to aid in breastfeeding as well as helping your baby to latch on and nurse. Some babies will acquire a taste for garlic while others may not enjoy it. Try cooking with garlic or adding it to a side dish. Garlic comes in the form of capsules to those who cannot stomach the taste.
- Fennel. Fennel is a wonderful addition to any breastfeeding diet. This herb may actually benefit baby more than mom since it does pass through the breast milk as it eases digestion and helps to prevent colic. It contains estrogen like properties which aid in boosting milk supply. You may drink fennel as a tea or add fresh fennel to a salad or soup.
- 8. Oils/Fats. Healthy oils and fats are vital to a breastfeeding diet and should never be avoided. Babies not only need these fats to thrive, but breastfeeding mothers as well to produce a well-balanced milk supply. After all, breast milk is made up of primarily fats to nourish your baby’s growth. Try adding olive oil to your salad or eating salmon for dinner to boost your healthy fats for the day.
- Carrots. Carrots contain phytoestrogens & beta carotenes; two nutrients that lactating mothers need. This vegetable also helps regulate hormones as well. Try drinking a glass of carrot juice in the morning with your breakfast or steaming a side of carrots with your dinner.
- Ginger Root. This root is known to boost milk supply by contributing to milk letdown and allowing the milk to flow freely. Some mothers benefit from simply drinking Ginger Ale. Another way to use Ginger in your diet is to boil the root and make an herbal tea. Some mothers may also find it beneficial to add fresh grated ginger to salads or salad dressings. If you cannot stomach the taste of ginger root, you may take ginger in the form of a capsule.
There are also some herbs that have been known to have lactogenic properties! Here are some of the best ones:
Blessed Thistle
This herb increases breast milk while helping to alleviate mild forms of postpartum depression. It is a bitter herb (known as a digestive bitter), which is healthful for the liver and digestion. Although it is an effective herb for increasing milk production, it is no longer included in the Nursing Tea. Many customers found it to be too bitter and did not like the taste, therefore hesitated to use the tea. We do have Blessed Thistle available as a single herb in the tincture form.
Brewer’s Yeast
Brewer’s yeast is often recommended as a nutritional supplement during breastfeeding. It is used to increase the supply of breast milk, but it is also believed to help combat fatigue and fight off the baby blues! A good source of iron, chromium and selenium, brewer’s yeast also contains several B vitamins, though not B-12.
Alfalfa
This is a great herb for increasing breast milk production while providing the body with lots of good vitamins and minerals. It is very high in Vitamin K in particular, which helps to staunch bleeding. Many midwives encourage all their clients to take Alfalfa for at least six weeks before birth, and for several months afterwards, to help avoid hemorrhage at the birth, and to help the body recover and make plentiful breast milk afterwards. (Alfalfa is also an ingredient in the Nursing Tea/Nursing Tincture. Note: This herb is not recommended for use by those on blood-thinning medications due to its high levels of Vitamin K.
Fenugreek
This is perhaps the most widely known herb for stimulating the production of breast milk. Most mothers usually notice an increase in milk production after 24-72 hours within taking this herb. It stimulates the mammary glands because it contains phytoestrogens which are plant chemicals similar to the female sex hormone estrogen.
Mother’s Milk Tea
When I worked at GNC, postpartum mothers swore by this stuff and would buy it by the SHIPMENTS! This tea contains anise, fennel, and carraway-other herbs that have been linked with milk production-and makes a great addition to taking Fenugreek. Also, who doesn’t love a nice nightly tea? I know I do! This can be bought at your local GNC.
Goat’s Rue
Goat’s Rue is a powerful herb for stimulating milk production and increasing the flow of breastmilk. It has been shown to increase milk production by 50% in many cases, and may also stimulate the development of the mammary glands themselves. This herb is safe for use during pregnancy. This herb is one of the main ingredients of the Nursing Tea/Nursing Tincture. It can be used as a single herb by itself, or to use along with or to add to the Nursing Tea/Tincture when something a little stronger is needed.
Building Your Milk Stash
So, you wanna build a stash?
I started building my stash the moment I got home from the hospital and I am so glad that I did! I think that every mother (if able) should try to express at least 3-6 months’ worth of milk to tuck away in their deep freezers for safe keeping because you never know when you might need it! And if you don’t? You can always do the generous thing and donate to your local NICU (yes, you can actually do that!) and help another mother in need.
Here are some benefits to creating a milk stash:
- You will need some kind of stash when you are returning to work
- If you baby happens to start rejecting the breast, the pumped milk will come in handy
- You can use the milk for future recipes involving your baby as he or she grows
- If your breasts dry up or your milk production abruptly stops for whatever reason, you’ll still be able to give your baby your breast milk
- Your milk stash can last up to six months in a deep freezer (some people even arguing nowadays that you can store it up to one year!)
- If you are traveling away from your baby or need a night out
- If you are on special medication or needing to be hospitalized
- For peace of mind
When storing your milk, it is very important to follow certain rules. Here are some tips to swear by:
- Always date your milk bags with a permanent marker
- Stock from older milk to newer milk
- Use shoeboxes to store your milk more effectively in your deep freezer
- Store smaller amounts to reduce possibility of waste
- Follow safety guidelines such as the Medela chart below
When you are ready to use some of your stashed frozen milk, here are some ways to properly thaw the milk:
- Let thaw in a bowl of cool water
- Let thaw in the fridge overnight
- Can be thawed for up to 24 hours. If left out longer to thaw, discard immediately.
When the milk is to be heated up, here are some proper ways to doing so:
- Warm milk under running warm water or place in a bowl filled with warm water
- Immerse in a pan that has been heated on the stove, but do not boil the milk directly on the stove. Pull the pan off first and allow to sit for a minute.
- Use a bottle warmer following the manufacturer’s instructions
- DO NOT BOIL OR MICROWAVE
Breastfeeding Diet & Lactation Recipes
Diet plays a huge role in breastfeeding. Essentially, what you eat, baby is eating. Well, kinda. He or she is getting the nutrients from the food, that you absorb through eating, in their breast milk. Did you know that what you eat can actually influence their taste? This also is said to apply while in the womb, too!
At every meal, make sure to include three food groups. For every snack, include two food groups. This way, you will be well-rounded in your diet.
- Fruit: (at least 3 servings) One serving equals 1 medium whole fruit or 1/2 cup (a generous handful) of cut-up fruit (or juice)
- Veggies: (at least 4 servings) One serving equals 1 cup leafy greens or 1/2 cup (a generous handful) of cut-up raw or cooked veggies
- Dairy: (at least 3 servings) One serving equals 1 cup milk or yogurt or 1 1/2 ounces cheese (about the size of your thumb)
- Whole Grains: (at least 4 servings) One serving equals 1 slice bread or 1/3 cup grains (a palm-size handful)
- Lean Protein: (at least 3 servings) One serving equals 1 ounce of nuts (a small handful), 2 tablespoons peanut butter (golf-ball size), a 4-ounce (palm-size) portion of meat or fish, or 1/2 cup beans (a generous handful)
- Treat: (1 serving of a favorite food every two or three days) Check nutrition labels for serving sizes
Sample Breastfeeding Diet Menu
Breakfast
1 egg, boiled or poached
2 slices whole grain toast with 2 teaspoons butter
1 serving fruit or 1/2 cup fruit or vegetable juice
1 cup non fat milk
Morning Snack
1 cup cereal
1/2 cup non fat milk
1 serving fruit
Lunch
Sandwich: 3 ounces turkey, 1 bagel and 2 teaspoons mayonnaise
Large salad with assorted veggies and 2 tablespoons low fat dressing
1 cup nonfat milk
1 serving fruit
Afternoon Snack
Muffin with 1 tablespoon peanut butter
1 serving fruit
Dinner
3 ounces beef or poultry
Large salad with 2 tablespoons low fat dressing
Cooked broccoli – 1 cup
Sweet potato – 1
Before Bed (or Midnight) Snack
1 cup cooked oatmeal or 1 cup dry cereal
1/2 cup non fat milk
Here are a few yummy treats that you can get away with because they have been known to promote lactation:
Banana Oat & Flax Lactation Pancakes:
Ingredients
- 1 cup rolled oats
- 3/4 cup Silk almond coconut milk
- 4 tsp flax seeds
- 1 banana
- 1 tsp vanilla
- 1 tbsp cinnamon
- 1 tbsp coconut oil (for the skillet)
Directions:
- Combine all ingredients in a blender-I use my Blendtec because it makes batter.
- Pour onto a heated skillet, with melted coconut oil.
- Heat each side for about two-three minutes. Flip. Repeat.
- Apply fresh fruit, nuts, or organic pure maple syrup!
Strawberry Oat Lactation Smoothie Recipe:
Ingredients
- 1 cup strawberries
- 1 cup ice
- ½ cup Almond Milk
- 1/4 cup Oats
- 1 Tsp Flax Seeds
- 1 Tbsp Brewer’s Yeast
Directions:
- All all ingredients into blender and blend on med to high until it has reached your desired texture.
Lactation Cookie Recipe:
Ingredients:
- 1 cup butter (2 sticks, softened)
- 1 cup white sugar
- 1 cup brown sugar
- 6 tablespoons water
- 3 tablespoons flaxseed meal
- 2 large eggs
- 1 teaspoon vanilla
- 1 teaspoon cinnamon
- 3 tablespoons Brewer’s yeast
- 2 cups all purpose flour
- 1 teaspoon baking soda
- 1 teaspoon salt
- 3 cups thick cut oats
- 1 bag chocolate chips
Directions:
- Preheat oven to 350.Mix flaxseed meal and water, set aside 3-5 minutes.
- Cream butter and sugar with electric mixer.
- Add eggs.
- Stir flaxseed mix into butter mix and add vanilla.
- Beat until well blended.
- Sift: dry ingredients, except oats and choc chips.
- Add butter mix to dry ingredients, beat well.
- Stir in the oats and then the choc chips.
- Using cookie scoop, drop on baking stone.
- Bake 11-13 minutes.
Lactation Boosting Funky Monkey Milkshake:
Ingredients:
- 1 frozen banana
- 1/4 cup quick oats
- 2 tbsp peanut butter
- 2 tbsp flax seed
- 2 tablespoons chocolate syrup
- 3/4 cup almond milk
- 2 cups ice
Directions:
- In a blender, at the oats and give it a quick pulse or two.
- Add remaining ingredients, except ice, and blend until well combined.
- Add 2 cups of ice until well blended.
- Enjoy with a thick straw or a spoon!
Apple Pie Lactation Oatmeal:
Ingredients
- 1 cup water
- 2 tbsp flax seeds
- 1 tbsp brewers yeast
- 1 apple chopped into cubes
- 2/3 cup oats
- 1 cup almond milk
- 1 tbsp cinnamon spice
- handful of pecans or walnuts (optional)
Directions
- Combine the water and apples in a saucepan.
- Bring to a boil over high heat, and stir in the rolled oats, yeast, flax, and cinnamon.
- Return to a boil, then reduce heat to low, and simmer until thick, about 3 minutes.
- Spoon into serving bowls, and pour milk over the servings.
Breastfeeding Obstacles & How to Overcome Them
When it comes to breastfeeding, most mothers will vouch that there can be some issues that come along with it. I won’t sugar coat my experience-my nipples hurt like HELL for at least 3 months. Since I had started off on the wrong foot with nursing, my son still just loved to only latch onto the nipple and not the entire areola! Luckily, I did not have any more issues (besides the poor latch) throughout my beastfeeding journey… well, except for when my little one got his first two teeth. OUCH!

Here are a few of the most common breastfeeding related issues and how to overcome them:
Clogged Ducts: These are not fun! Clogged ducts are when one of your milk ducts basically become clogged and cannot relieve itself of the milk. Think of a bathtub and a stopper. The bathtub is filled to the brim and the water cannot go down the drain to empty the tub. Your breast is the same exact way. The duct will be very sore or tender to touch. The best thing to do with a clogged duct is to feed on the effected boob, though it may be painful-you’ve got to get that duct open and back to work! You can also try a heat massage using a warm compress in the shower. You may even try dangle feeding, such as below (though I promise you do not have to do a plank as I did).
Thrush: Thrush is caused by an excess of fungus that lives off and feeds on breast milk. It is caused by Candida, which you might have heard before as it is also responsible for yeast infections. Most women develop thrush after using antibiotics and their babies can get it too. It is also caused by an area staying moist for too long of a time period. Easy way to check your baby is to check its tongue-usually a thick, white patch that cannot be easily scraped off is a result of thrush! It may even appear as little white spots within the mouth. Your baby can also get thrush as a result his bottom being too moist. My son got this constantly and we had to see a pediatrician for this to get Nystatin cream. Mama, you can get thrush too! Check your nipples from time to time-any signs of bleeding, rash, redness, pain, etc can be a result and you will need to be treated for it.
Low Milk Supply: Many women worry about this happening and sometimes it does happen here and there during your breastfeeding journey. The best way to notice is your supply is running low is to check your baby’s weight. If his or her weight is right on target for their age, then mama you are doing a great job and are producing enough! However, if your baby is losing weight and you truly aren’t making enough milk, first check the latch to make sure it’s correct. Don’t forget to offer both breasts and allow baby to finish when he or she is falling asleep. Let formula become your last resort.
Oversupply of Milk: Having an oversupply of milk is about as common as not having enough. It can actually be frustrating for the baby as your “let-down” nearly drowns him or her during each feed. What to do? Slow down your feedings. Offer only one boob per meal. Then turn around and feed off the same boob. With time, your milk will even out-I promise! It just takes a few months to get into the swing of what your baby is demanding, in order to create the exact supply.
Sore Nipples: Sore nipples are usually caused by a poor latch and is actually the #1 problem that breastfeeding mothers experience today. Babies do not come pre-programmed as professional latchers-we actually have to teach them how and guide them, as mentioned in Chapter One. It is normal for your nipples to hurt for a few days, but any prolonged pain needs to be addressed with a lactation consultant immediately! The only way to fix this issue is by teaching your baby how to latch on fully and correctly, by taking nipple and aerola into their mouth.
Nursing Strike: A nursing strike is, when out of the blue, your baby does not want to take the breast. You may start to worry that your baby does not want to breastfeed anymore, but this is usually NOT the case. When babies start acting weird and refusing your breast milk, there is usually an underlying problem being missed such as thrush, an ear infection, a virus, etc. This is their way of telling you, mom, that he or she is not feeling well and that there is something wrong. When in doubt, always take a trip to the doctor’s office or ER-to be on the safe side.
Engorgement: Engorgement is another very common issue that a lot of breastfeeding moms deal with on a regular basis. Most of the time, it is mothers who do not have time to pump or are away from their babies during the day that face this type of issue. This also happens as soon as your milk comes in shortly after birth! Your breasts may be warm to touch, throbbing with pain, and overall HUGE. The #1 way to resolve engorgement is by expressing that milk ASAP or else it can lead to mastitis, a potentially serious breast infection, or clogged ducts. Engorgement can be a sign that your baby isn’t getting enough milk so, as always, check your latch or talk to a lactation consultant. Otherwise, a great way to relieve engorgement is cold and warm therapy. Using a cold ice pack will help with the swelling and apply heat will help open up those ducts some. Lots of women I know will take hot showers to relieve the pain and they tell me all the time how the milk will immediately come flowing out! You can also massage your breast to help ease the pain as well. This usually resolves itself. When in doubt, see a doctor!
Mastitis: This is the bigger, here. Mastitis is a breast infection and occurs when the milk has been engorging your breasts for way too long. It causes fever or flu like symptoms and needs to be treated by antibiotics right away because it usually does not improve on its own. Your breasts will be very hot to touch and appear red. Some women even report a yellowish fluid leaking from the breasts-a sign of infection. If you think you have Mastitis, see a doctor right away so you can begin treatment. Other things that will help including breastfeeding or pumping the affected breast, massage, and cold/warm compress.
Breastfeeding & Supplementation
A lot of women tend to have plenty of questions and concerns revolving around the use of supplements during breastfeeding. As with anything else, you should always consult with your physician before ever trying a new supplement. I do take a few supplements on a daily basis that I will certainly share with you, but, by no means, does that mean what works for me may work for you. Every single human body is so genetically engineered differently so always take caution!
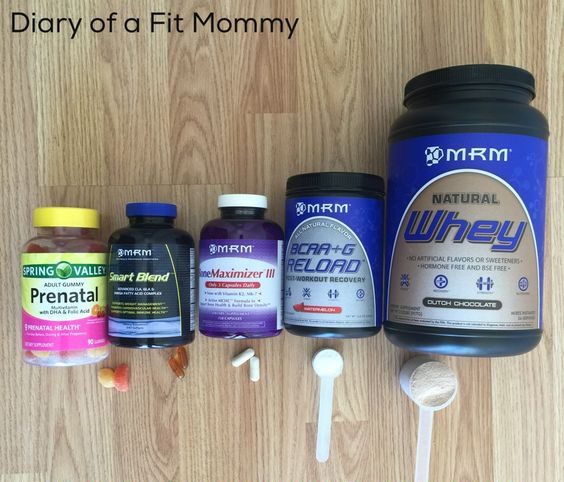
First and foremost, a good multivitamin is a MUST have. It will also help cover any bases for you as far as nutrients goes, but should never be substitued for a healthy diet packed with vitamins and minerals.
Secondly, a whey protein powder that is safe for you and baby is key. Currently pregnant, I use MRM’s Natural Whey which is completely natural and isn’t filled with all of those yucky chemicals that you find in most whey powders. This protein is also safe for breastfeeding mommies as I will continue taking it to get in shape post-baby. Take 40% off all MRM supplements with code SIA at checkout! Using a whey protein will deliver a good bit of protein super quickly to your muscles after or during your workout for the ultimate recovery.
Thirdly, a fish oil supplement is perfect for you because it supports a healthy metabolism and fat loss during your workouts, as well as being a natural appetite supressant! I personally use MRM’s Smart Blend. It is safe for breastfeeding and I love knowing that it helps my baby. Again, in case you missed the coupon code, take 40% off all MRM product with code SIA!
Fourth, a calcium supplement is a great idea for breastfeeding mommies! Even pre-natal vitamins do not contain 100% of your daily calcium so you will need something extra. Most dairy products contain a lot of calcium and you can also get it from broccoli, baked beans and some nuts. I use MRM’s Bone Maximizer!
Lastly, an optional, but goodie for workout recovery and muscle building during pregnancy are BCAA’s. I use MRM’s BCAA Reload as its 100% natural and safe for pregnancy and breastfeedding. BCAAs are the building blocks of muscle and helps to reduce muscle soreness after a workout while also increasing your strength.
Weightloss & Breastfeeding
I always get emails coming in regarding caloric & nutritional intake requirements while breastfeeding and also what I’ve been eating and how many calories I’ve personally been taking in. I’ve also had a few questions regarding postpartum weight loss while trying to breastfeed, which is a great topic because so many women are always wanted to get back into shape shortly after giving birth.
When I was pregnant, I was eating around 2,300 calories daily for mostly all 3 trimesters. Some days, I would even eat up to 2,500-especially in the third trimester when I had a lot less energy and was hungrier! While breastfeeding, you need 500 extra calories tagged into your daily value to make up for the amount of calories being burned throughout the day from feeding your baby. Isn’t it crazy that breastfeeding burns that much!
To figure out the minimum of daily calories that you specifically need when breastfeeding, you must first figure out what your baseline daily caloric intake is. To do so, there are tons of calculators out there to give you a good ballpark estimate, such as this one: http://www.acefitness.org/acefit/healthy_living_tools_content.aspx?id=4
My number was in the 1800s for my minimum daily intake. If I go below this number, I could risk losing my milk production. So I took this number and automatically tagged 500 onto that, and that basically lets me know how much I can consume on a daily basis.
But wait-what if I am working out? Here’s where the numbers get tricky because everyone is so different-so is every internet calculator you find. Seeing a dietician is the best thing you can do throughout your pregnancy and postpartum to find the perfect number for you, but if you want to figure it out on your own, I suggest going by the Breastfeeding calculator’s minimum requirement, then adding the extra 500, and then using something such as MyFitnessPal to track not only your calories being consumed, but your calories from activities that are being burned-this way, you can eat back what you burn OR make sure you do not dip below the minimum caloric requirement that you need for Breastfeeding, ensuring you have enough for lactation.
Make sense?
Next topic, postpartum weight loss while breastfeeding. This tends to be slightly controversial because in order to lose weight, it usually means cutting back calories, right? Right! But, that’s not a bad thing.
Some postpartum breastfeeding women will notice that they keep a bit of a softer figure while they are lactating. This makes sense because you are eating to keep up with those lost calories. Is it possible to lose weight and still breastfeed? Absolutely! So, how?
Remember those calculators mentioned above? Take the minimum amount of calories needed to ensure lactation and tag on that 500 extra calories that you may consume. Workout and burn those calories-but don’t let your daily intake slip below the minimum line. There you have it! Is it really that simple? Well, it depends on you. Everybody is different. You may notice a change in your milk production though if you decrease your calories or you may still be golden. One thing I would recommend is no drastic drops in calories-slowly burn more at a time. When in doubt-speak to a nutritionist or a dietitian!
I will be building muscle and toning up when given the clear in a month so I personally won’t be lowering my calories to lose weight. I will be upping my calories to put on that lean muscle and to get rid of my softness that I have. I have cellulite. I have a little flab. Since I have birth, my butt is virtually FLAT! Lol, I miss my preggo behind. I promise, I am human and I am NOT perfect at all.
No matter what your weight loss or weight gain goals are, we are all in this together. Breastfeeding is the best thing you can give your child (if you are able) and losing a few pounds isn’t worth the risk in losing your milk production so take it easy, listen to your body, and definitely consult with your doctor.
Breastfeeding & the Working Mom
Some of you ladies know that I work from home. I realize that not many women actually get that luxury (sometimes it is a luxury, other times I want to pull my hair out) and as soon as the maternity leave is up, back to work they go.
And the number one fear is “OMG what do I do now?”
No worries! Women have been pumping and working for many years now and you are not alone. I have tons of friends who are working mothers and are pumping away at every chance that they get. How do they do it? I will explain.
There are certain tools and tips that will make your life a whole lot easier when you make the smooth (hopefully) transition back to work. The hardest part about it will probably not having your baby around you all day (which can sometimes be a blessing of relief- take my word for it). It simply takes lots of preparation and planning-mentally and physically.
Here are 4 steps to successfully pumping as a working mother:
- Get your essentials together. You will need to make sure that you have all necessary tools available to make sure you pump successfully on the go. The very bare essentials are:
- an electric pump (double electric is best)
- a hands-free nursing bra (ok so this may be a bit optional but if you are a desk worker; this is the way you can type and pump)
- bottles & bags for storage
- a bottle cooler and/or ice pack (this will help keep your pumped milk cool on the way home)
- extra pumping parts, bottle brush, and a disinfecting soap (this is considering you have a kitchen or sink within your workplace.)
- Begin pumping & building your stash during maternity leave. (see Chapter 6)
- Establish a routine or make your plan of attack. We discussed routines in chapter four. Depending on your job, your break times, and your busiest times will determine which pumping routine or schedule is best for you. As a rule of thumb, to keep your supply healthy and running, it is a good idea to try and pump once every 4 hours-at least. To mother’s who are working an 8 hour day, yep, that means you are pumping during your lunch break.
Here is a little breakdown of how your pumping should go on a normal working day:
- 5am-6am: Wake and breastfeed your baby.
- 7am-8am: Pump before heading out the door (even if it’s for a few minutes)
- 11am-12pm: Lunch break/Pumping
- 4pm-5pm: Pump a little before leaving work.
- 5pm-6pm: Breastfeed your baby for the rest of the night (unless you want to pump before bedtime or wake up at night to pump)
For mothers who need to pump more often, please keep in mind that most employers will allow a couple of 10-15 minute breaks during your workday and this is actually a perfect amount of time to get to pumping-especially with a double electric in which you are pumping both breasts at the same time!
However, some states still do not protect nursing mother’s right to express milk so if an issue arises, please talk to your Human Resources Manager if you have any questions. Also, talking to your employer before taking your maternity leave to sort things out is also a good idea. Let them know your desire to pump on the job and get a feel of what to expect and your employer’s feelings on the topics then-this way you won’t be blind sighted when you return to work.
Be confident. Your feelings truly will affect your milk supply and your ability to pump effectively. You have to relax in order for the milk to flow so do not (at least try not to) let any stress get the best of you! You are doing your very best for your baby and family and that is all that matters. It just takes some time.
My Nursing Essentials
What you need for nursing and pumping varies from mommy to mommy, but I have my personal list of nursing MUST HAVES that I always make sure to have on hand:
- 1 Double Electric Pump
- 1 Manual Pump
- Extra Pump Parts
- Milk freezer/storage bags
- Bottles of different sizes
- Extra nipples and bottles
- Sterilizing bags for the microwave
- Bottle Warmer
- Bottle Brush
- Bottle drying rack
- Lanolin
- Bamboo nursing pads (washable)
- Portable insulated bottle bag
- Unlimited burp cloths
- Mother’s Milk Tea
- Boppy pillow
- Water! H2O!
- Oats
- Nipple Shields
- Lansinoh Soothies gel pads (ahhh relief!)
- Lansinoh Therma-Pearl 3-in-1 Breast Therapy (You are going to love this product)
- 2 nursing sports bras (Cake Lingerie)
- 5 regular nursing bras (HotMilk Lingerie)
- 2 sleeping nursing bras (Basics by Bravado)
- 2 nursing pajamas (Bellefit)
- About a whole wardrobe of v-necks and nursing-wear. (just kidding, but no, seriously)
You will find that some of this stuff is not completely necessary-it’s just simply nice to have on hand. You will find your very own items that are essential to you, with time!
Conclusion
As you can see, there are tons of information that goes along with breastfeeding and pumping. At times, it can be totally overwhelming-especially when you have nobody to turn to. I hope that this post has helped you on your journey to becoming one badass breastfeeding & pumping mama! If you have any questions at all, feel free to contact me or leave a comment.
Your trainer and friend,